Why belly fat deserves attention
After the festive season, many people notice extra weight around their middle.
For most, it feels like a temporary inconvenience. But doctors say belly fat can mean much more than just a change in appearance.
A growing body of medical evidence suggests that weight carried around the abdomen may be linked to serious health risks that aren’t always visible on the surface.
Weight loss is often framed around aesthetics.
Abs, beach bodies, and clothing sizes dominate the conversation.
But according to Dr Amir Khan, focusing purely on looks misses the real issue.
The goal, he says, should be better health — not chasing an ideal body shape.
Not all fat behaves the same way in the body.
Dr Khan explains there are two main types: subcutaneous fat and visceral fat.
Subcutaneous fat sits just beneath the skin.
It’s the type you can pinch and is generally less harmful.
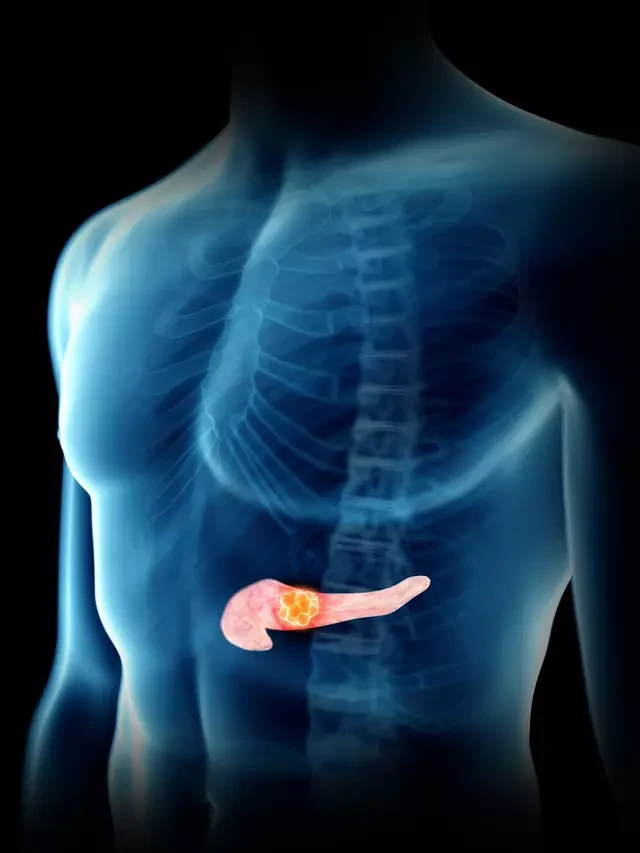
Visceral fat, however, is stored deeper in the abdomen, wrapped around vital organs such as the liver, pancreas, and intestines.

Why visceral fat is more dangerous
Visceral fat is strongly linked to metabolic and cardiovascular disease.
Higher levels are associated with type 2 diabetes, high cholesterol, heart disease, and increased inflammation in the body.
What’s often overlooked is that someone can appear slim overall but still carry high levels of visceral fat, particularly around the stomach.
That matters because visceral fat interferes with how the body regulates blood sugar, hormones, and cholesterol.
Dr Khan warns that belly fat can be an external sign of internal stress on the body.
Excess abdominal fat may indicate insulin resistance, fatty liver disease, or elevated cardiovascular risk — even before symptoms appear.
This makes belly fat less about appearance and more about long-term health outcomes.
While visceral fat poses greater risks, it also responds more quickly to lifestyle changes.
Dr Khan notes that this type of fat is metabolised faster than subcutaneous fat.
Because it’s more biologically active, the body can reduce visceral fat relatively quickly through improved movement, nutrition, sleep, and stress management.
What helps reduce abdominal fat
According to guidance from the Cleveland Clinic, reducing visceral fat typically involves a combination of habits rather than a single solution.
Regular physical activity that raises heart rate is key.
Strength training also plays a role by improving muscle mass and metabolic health.
Nutrition matters as well.
Balanced meals, reduced ultra-processed foods, and limiting alcohol intake are all linked to lower abdominal fat levels.
Quality sleep and stress reduction are also important.
Chronic stress raises cortisol levels, which can promote fat storage around the midsection.
Doctors stress that the aim shouldn’t be rapid weight loss or extreme dieting.
Instead, sustainable habits that support overall health tend to deliver the most meaningful results.
What’s often overlooked is that improving metabolic health can happen even without dramatic changes on the scale.
Small reductions in visceral fat can significantly lower disease risk over time.
When to seek medical advice
Carrying belly fat doesn’t automatically mean someone is unhealthy.
But sudden changes in weight distribution, combined with fatigue, blood sugar issues, or a family history of metabolic disease, may be worth discussing with a healthcare professional.
Early awareness allows people to take preventative steps long before serious illness develops.
Health Disclaimer
This article is for informational purposes only and is not intended as medical advice. Always consult a qualified healthcare professional before making any changes to your health, diet, or treatment.
Featured Image Credit: Getty Stock
Topics: Health, Instagram, Weight loss