As winter illnesses surge, many people expect to battle coughs, fevers, and fatigue. For one mother in Wales, those familiar symptoms nearly proved fatal.
A 27-year-old woman has now shared her story to warn others after what she believed was the flu turned out to be sepsis, a life-threatening medical emergency that left her unresponsive in bed.
A Routine Illness That Was Anything But
Roberta Alisauskaite, a mother of two from Carmarthenshire in South West Wales, said she first began feeling unwell in October. Like many during colder months, she assumed she had picked up a seasonal bug from work.
At first, the symptoms felt manageable. She described feeling under the weather, run down, and feverish — all signs many associate with flu or a heavy cold.
What she didn’t realize was that her body was already fighting something far more dangerous.

Symptoms Escalated Rapidly
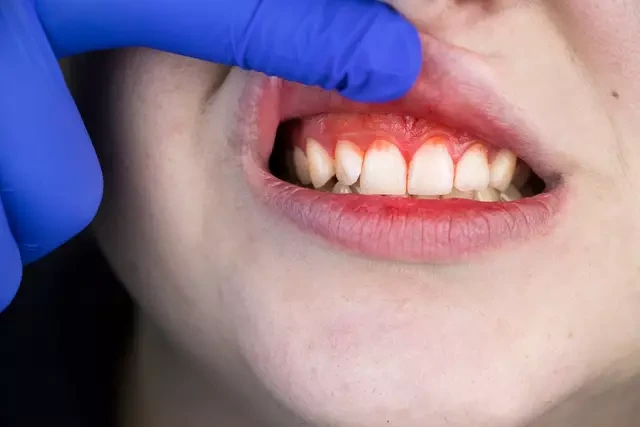
Alongside flu-like symptoms, Alisauskaite was dealing with an abscess linked to one of her wisdom teeth and had been taking antibiotics. Within days, her condition deteriorated quickly.
She developed violent shaking, an uncontrollable fever, and a worsening cough. Her temperature spiked, her breathing became labored, and confusion began to set in.
Despite turning on the heating and wrapping herself in blankets, she said her body alternated between intense chills and overwhelming heat.
Found Unresponsive by Her Children
The situation reached a terrifying turning point when Alisauskaite was found upstairs by her two young children. She was unresponsive and struggling to speak clearly.
She later explained that she was slurring her words and could no longer make sense, a moment she says deeply traumatized her children.
An ambulance was called, and she was rushed to hospital, where doctors carried out urgent tests.
The Real Diagnosis: Sepsis
Instead of flu, doctors determined she was suffering from sepsis, a condition caused by the body’s extreme response to an infection.
Consultants told her she had gone into septic shock, a severe and potentially fatal stage where blood pressure drops dangerously low and organs can begin to fail.
According to health authorities, sepsis requires immediate treatment. Delays can dramatically increase the risk of long-term complications or death.

Why Sepsis Is Often Missed
Medical experts say sepsis is frequently mistaken for flu, especially in its early stages. Fever, muscle pain, chills, and exhaustion can feel deceptively familiar.
What’s often overlooked is how quickly symptoms escalate. Confusion, breathlessness, uncontrollable shivering, and changes in speech are red flags that demand urgent medical attention.
The NHS and other health bodies stress that there is no single symptom of sepsis, making awareness crucial.
A Message for Other Parents and Families
Now recovering, Alisauskaite has spoken publicly to encourage others not to ignore worsening symptoms.
She says she never imagined a common illness could leave her fighting for her life, and she urges parents in particular to trust their instincts if something feels wrong.
Her story comes as winter illnesses place extra pressure on healthcare systems, a time when serious infections can easily be misjudged.
When to Seek Urgent Help
Health experts advise seeking immediate medical care if flu-like symptoms are accompanied by confusion, difficulty breathing, persistent vomiting, extreme shivering, or sudden changes in consciousness.
Early treatment saves lives. Acting quickly can mean the difference between recovery and devastating outcomes.
Featured Image Credit: Kennedy