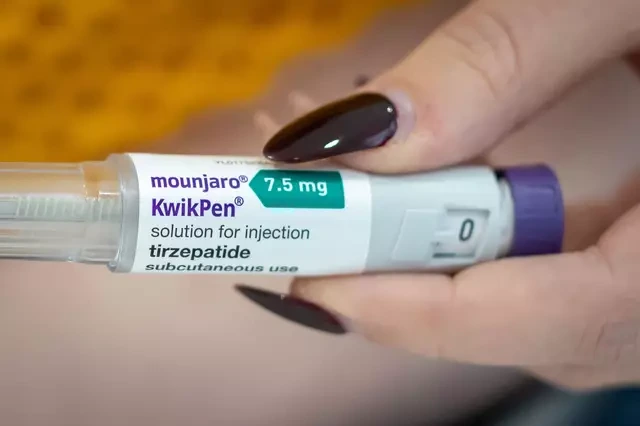
If you’ve spent any time in weight-loss jab communities online, you’ve probably seen it mentioned: the “golden dose.”
The idea is simple. People notice there’s still liquid left in a Mounjaro pen after the fourth injection, and some try to use it as an extra bonus shot.
Here’s the problem: experts say that leftover liquid is not an extra dose. It’s overfill, and using it can create avoidable risks.
What people mean by the “golden dose”
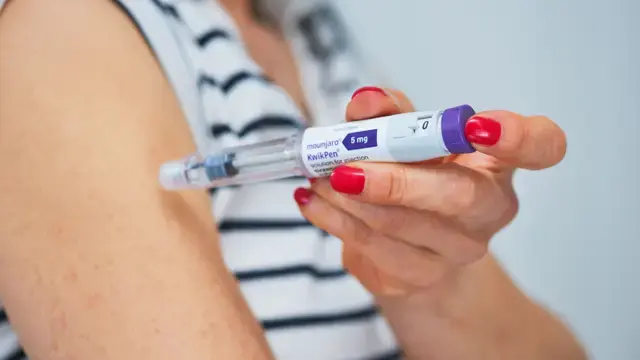
Mounjaro (tirzepatide) is a prescription injection used for specific medical indications, and many people now associate it with weight-loss support under clinical guidance.
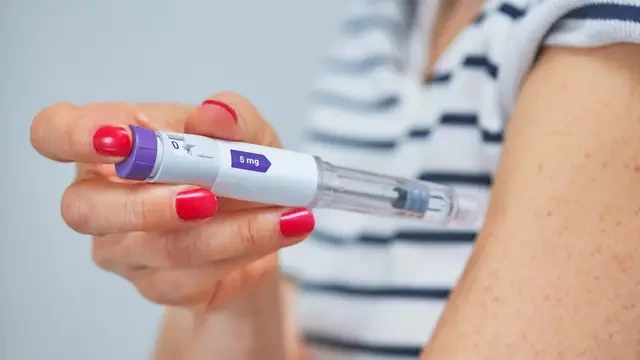
Each pen is designed to deliver four set doses. The device also includes a small amount of extra liquid. Manufacturers typically build in overfill so the pen can reliably deliver full, accurate doses each time.
That leftover liquid may look like “one more,” but it isn’t measured as a safe or consistent fifth dose.

Reason 1: You can accidentally underdose and stall progress
When someone tries to stretch a pen, the first risk is surprisingly the opposite of what they expect.
If you start “saving” or pulling medication differently, you can end up taking less than your prescribed amount across multiple weeks. That matters because these treatments rely on steady dosing schedules to maintain predictable effects on appetite and blood sugar regulation.
People often blame the medication when results slow down. But inconsistent dosing can also explain why hunger cues return earlier than expected, or why progress feels uneven.
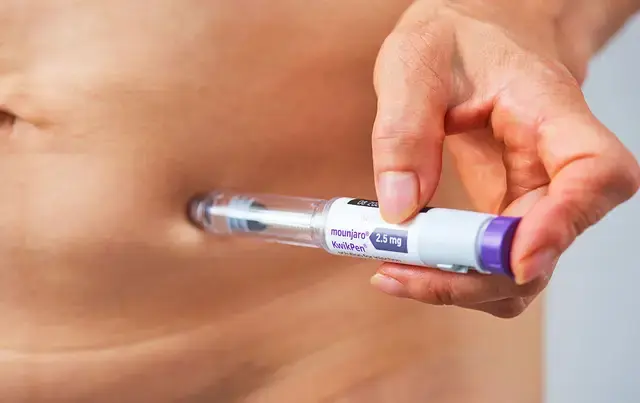
Reason 2: You can accidentally overdose and feel very unwell
Some people see the extra liquid as a clever workaround, especially when access or cost feels stressful.
But pens are not designed for precision outside their intended use. When you attempt to extract leftover medication, you don’t know exactly how much you’re drawing up.
Taking more than prescribed can increase the chance of intense side effects. With GLP-1-related medications, that can include severe nausea, vomiting, diarrhea, and dehydration. In rare cases, serious complications can occur, and clinicians take those risks seriously.

Reason 3: You may raise infection risk by using a pen outside its design
There’s also a practical safety issue that gets overlooked in social posts: sterility and storage.
Once you start using a pen in ways it wasn’t designed for, you increase the chance of contamination. That may raise the risk of injection-site irritation or infection.
Medication stability can also become an issue if a pen has been stored incorrectly or used beyond the recommended time window after first use. If the product degrades, it may become less effective, even if it looks normal.
If you notice redness, swelling, warmth, drainage at the injection site, fever, or you feel generally unwell after an injection, you should treat it as a reason to seek medical advice promptly.
Why “leftover” doesn’t mean “extra”
It’s easy to assume that if liquid remains, it must be usable. But device overfill exists to ensure accuracy, not to provide a hidden fifth dose.
That’s why the safest approach is also the simplest: use the pen exactly as directed and follow the dosing plan your clinician set for you.
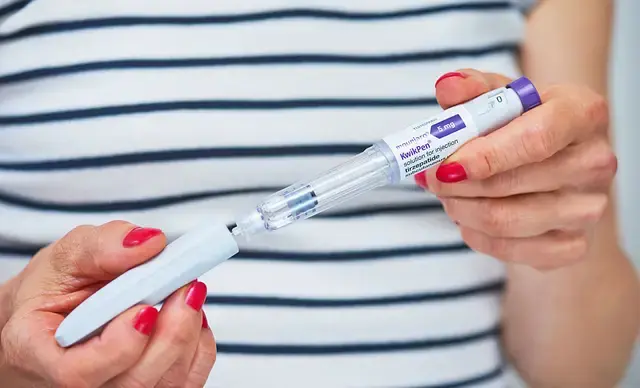
What to do if you’re worried your dose isn’t working
If you feel hungrier again, your weight loss slows, or side effects feel unmanageable, the answer usually isn’t to improvise with your pen.
A qualified healthcare professional can assess whether your dose needs adjustment, whether side effects require a slower increase, or whether something else is affecting your results. Organizations like the NHS, CDC, and Mayo Clinic consistently emphasize medication safety, correct use, and clinician oversight when it comes to prescription treatments.
Featured Image Credit: Peter Dazeley/Getty Images