Kidney disease rarely arrives with a dramatic warning. For many people, it builds quietly in the background until daily life starts to change in ways that feel easy to explain away.
That’s one reason health experts keep raising the alarm as chronic kidney disease (CKD) climbs the global rankings of major causes of death. According to the World Health Organization, the top 10 causes of death accounted for more than half of all global deaths in 2021, and kidney disease appeared among them for the first time.
What chronic kidney disease actually is
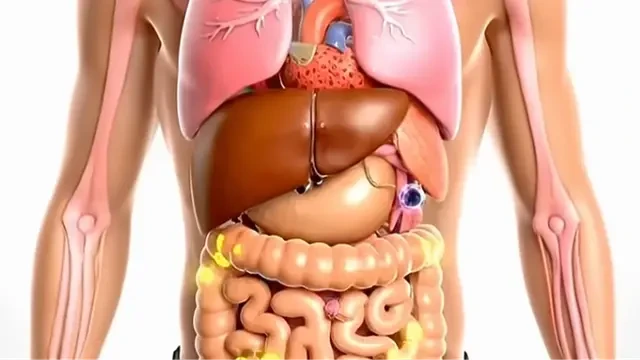
CKD is long-term damage to the kidneys that reduces how well they filter waste and extra fluid from the blood.
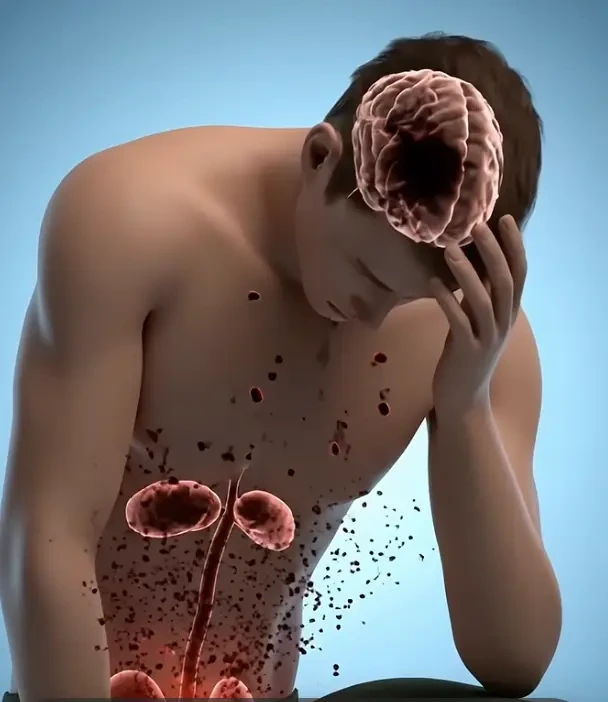
When kidney function drops, harmful waste and fluid can build up in the body. Over time, that can contribute to serious complications, including cardiovascular problems, and can become life-threatening.
Public health agencies like the CDC also warn that many people live with CKD without knowing it, which makes early detection a major challenge.
Why early symptoms are often missed
In the early stages, CKD may cause no noticeable symptoms at all. Some health authorities note that the body can cope with a significant loss of kidney function before clear signs show up.
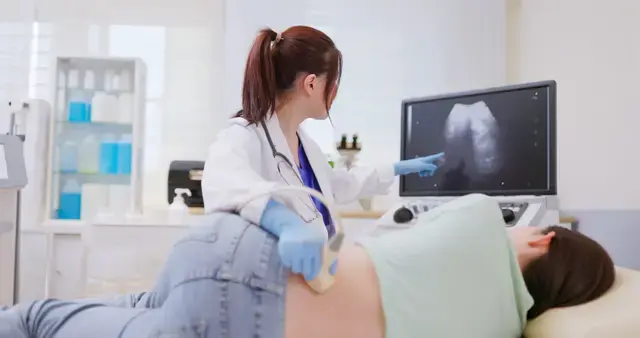
That means a diagnosis often happens during blood or urine testing done for another reason. It can feel surprising, especially for people who still feel “fine.”

Subtle changes that can show up first
When symptoms do appear, they can be vague and easy to blame on stress, age, or a busy routine.
People may notice fatigue that doesn’t match their sleep, a general sense of low energy, or trouble concentrating. Some report changes in appetite, including eating less than usual or unintentional weight changes.
Sleep can also shift. Some people experience restless sleep or insomnia, while others feel unusually sleepy during the day.
Swelling and fluid retention
One of the more visible warning signs is swelling in the ankles, feet, legs, or hands.
This can happen when the body holds onto extra fluid. It may come and go at first, which makes it tempting to ignore, especially if it seems linked to sitting for long periods or hot weather.
Some people also experience shortness of breath, which can have many causes. In CKD, it may relate to fluid balance issues or associated complications.

Changes in urination
Bathroom habits can change as kidney function declines.
Some people notice they urinate more often, especially at night. Others see foamy urine, which can signal protein in the urine, or they may notice blood in the urine.
These changes don’t automatically mean CKD, but they are often listed by health authorities as signs worth taking seriously in a medical setting.
Other symptoms that can develop later
As CKD progresses, symptoms may become harder to ignore.
People may experience nausea, headaches, muscle cramps, itchy skin, or a general feeling of being unwell. Some develop anemia, which can worsen fatigue and weakness.
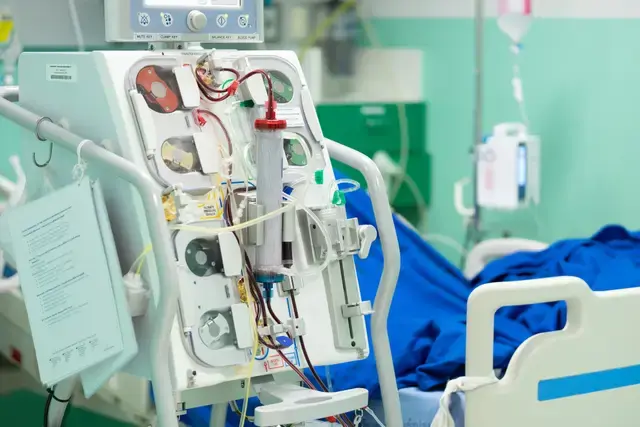
In advanced stages, the condition can progress to kidney failure, also called end-stage renal disease. At that point, treatments may include dialysis or a kidney transplant, depending on the person’s situation.
Why risk is rising
Researchers and public health agencies often point to overlapping drivers: high blood pressure, high blood sugar, and higher body weight can increase CKD risk. Population aging can also raise overall case numbers because kidney function naturally declines with age for many people.
What’s often overlooked is how “silent” the early phase can be. When a condition hides until it becomes severe, it tends to be diagnosed later and treated later, too.
Featured Image Credit: Getty Images/m-gucci
Topics: Health, NHS, US News, World News