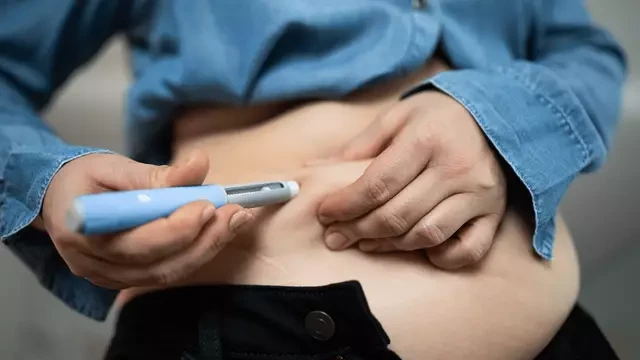
Weight-loss injections have gone from “something celebrities do” to something everyday people ask their doctors about.
But the first month can feel confusing. Some people expect instant results. Others worry the moment they feel nauseous that something is wrong.
Here’s what experts say you may experience in the first four weeks, and why the early phase is often more about adjustment than dramatic change.
Why the first month feels different for everyone
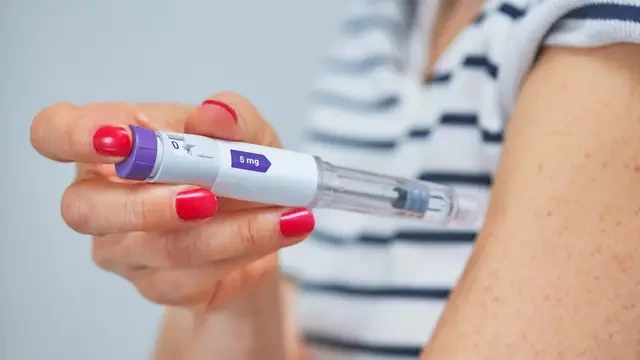
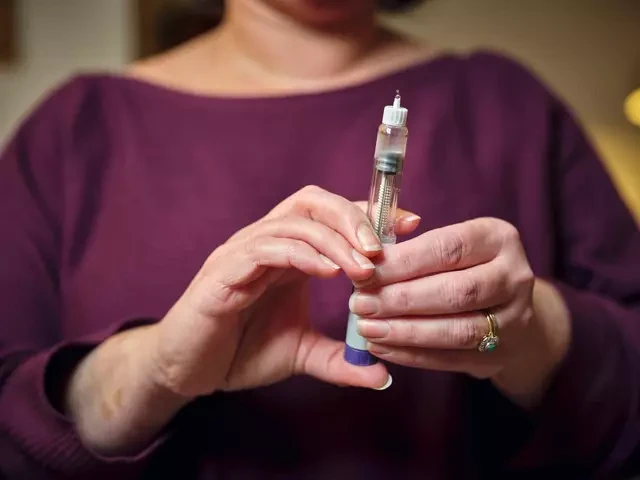
Medications such as Wegovy and Ozempic contain semaglutide, which works by mimicking a hormone involved in appetite and blood sugar regulation. That’s why changes often start in your gut and your hunger cues before you see big changes on the scale.
Your dose also usually increases gradually over time. So “week one” is not the same experience as later months on a higher dose.
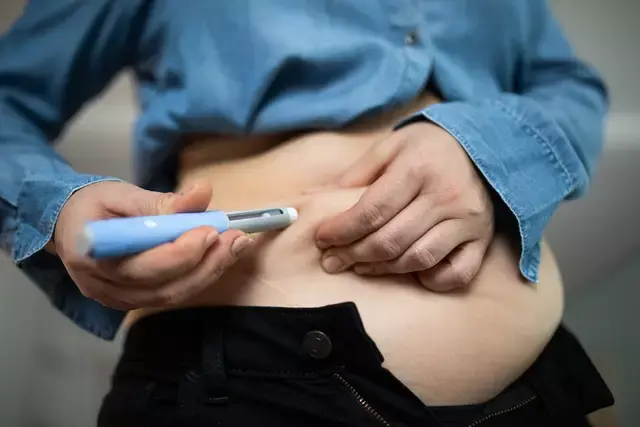
Week 1: Your body starts adjusting
In the first several days, some people notice appetite changes quickly. Meals may feel heavier, and it may become easier to stop eating sooner than usual.
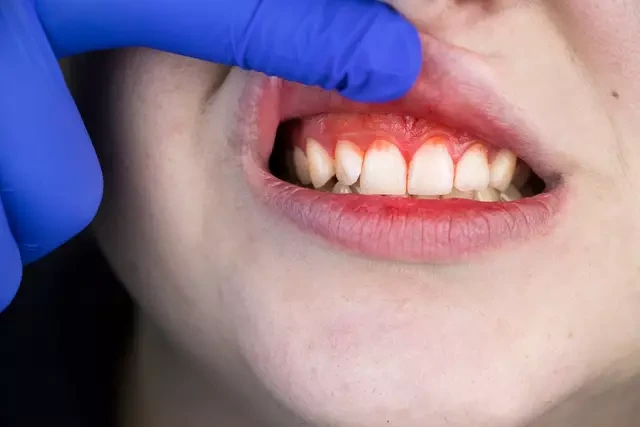
Side effects can also show up early. Nausea, vomiting, diarrhea, constipation, stomach discomfort, headache, and fatigue are commonly reported with semaglutide-based treatments.
Not everyone gets side effects, and intensity varies. For some, it’s mild and short-lived. For others, it can affect routine for a few days.

Week 2: Side effects may begin to settle
By week two, many people find their body starts to adapt. If you had nausea or digestive upset at the start, it may lessen as you learn what foods and meal sizes feel best for you.
This can also be the stage where patterns become clear. Some people realize they feel worse after large meals, greasy food, or eating too fast. Others notice they’re simply less interested in snacking.
If symptoms feel persistent or severe, that’s usually a sign to check in with a clinician, because dosing schedules and tolerability matter.
Week 3: Appetite signals often change more noticeably
Around the third week, some people describe a more consistent shift in hunger.
You may feel full sooner, think about food less often, or find it easier to stick to smaller portions. Semaglutide is associated with appetite reduction and changes in digestion that can make fullness last longer.
This is also where expectations can get tricky. Feeling less hungry does not automatically guarantee balanced nutrition. Even if you’re eating less, your food choices still matter for energy, protein intake, and overall wellbeing.

Week 4: Early progress can appear, but it’s not just the scale
By week four, some people see early weight changes. Others don’t see much movement yet, especially if side effects limited activity or if the dose is still low.
What’s often overlooked is that these medications are also studied for broader health effects. Wegovy, for example, is indicated for chronic weight management in certain patients and has evidence tied to cardiometabolic outcomes in specific groups.
If your prescriber is tracking metrics like blood pressure, blood sugar, or cholesterol, this is when “non-scale wins” may start to show up for some people—though changes can take longer and depend heavily on your starting point and overall health.
Why prices and access are part of the conversation now
Access has been a major barrier, and pricing shifts have kept the conversation in the spotlight.
In November 2025, Novo Nordisk announced it was lowering the self-pay price for Wegovy and most doses of Ozempic in the U.S. from $499 to $349 per month, alongside a limited-time introductory offer for new self-pay patients.
Even with changing costs, experts continue to stress that these medications work best when they’re part of a clinician-supervised plan, not a shortcut.
Featured Image Credit: Getty Images
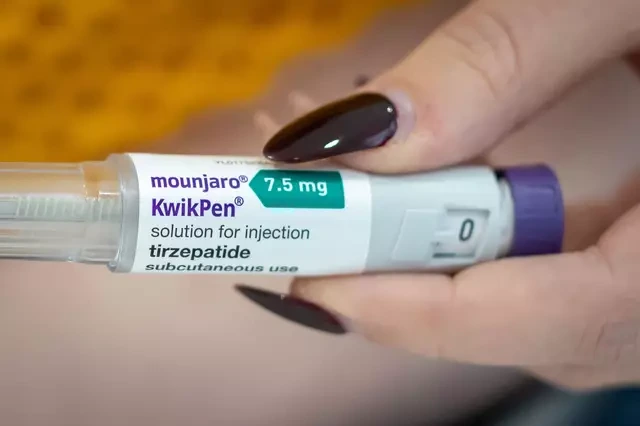
Topics: Health, Ozempic, Weight loss, Mounjaro